Often we treat pain without bothering with its definition. The majority of all pain patients recover quickly from their injuries; in fact, more than 90% will be fully functional within eight weeks simply because of the body’s ability to heal itself, regardless of treatment. However, it is the remaining people, who after months of persistent pain, become frustrated when medical examination does not yield a diagnosis and their doctors prescribe medications and therapies without producing lasting relief. The persistent physical discomfort of chronic pain can bring an individual to their emotional limit.
Pain is an entity that is commonly misunderstood because medical diagnosis traditionally presumes that pain is only a signal of tissue injury conveyed to the central nervous system. However, there are actually three distinct categories of pain: Nociception, Inflammation, and Neuropathy.
- Nociception: The immediate response conveyed to the brain, signaling tissue injury (noxious input). An example is the response from a slap to the skin.
- Inflammation: A local response to cellular injury resulting in redness, swelling, heat, pain and sometimes loss of function, and that serves as a mechanism initiating the elimination of noxious agents and facilitating the healing process.
- Neuropathy or Radiculopathic Pain: Ongoing pain with no obvious signs caused by a malfunction in the peripheral nervous system, leading to supersensitivity in the pain sensory system.
Neuropathy is a relatively new word, specifically referring to any functional disturbances or pathological changes in the Peripheral Nervous System (PNS); though it is often used incorrectly to describe the nervous system as a whole. It is imperative to distinguish these entities as separate, since they show different outcomes and presentations. The CNS is well-protected by the skull and the spine, unlike the often overlooked PNS, which is much more vulnerable to damage and denotes the greatest number of chronic pain cases.
Medical professionals are apt to treat pain in the first two categories, but are perplexed by pain that shows no sign of tissue damage or inflammation. Long-term pain can exist in ongoing nociception/inflammation such as a fracture or rheumatoid arthritis (treated with surgery or anti-inflammatory drugs), a psychogenic disorder such as clinical depression (treated with medication or counseling), or most commonly neuropathic pain (explained further below). Neuropathic pain has several indicators:
- There is pain in the absence of ongoing tissue damage.
- There is a delay in the onset of pain after a precipitating injury.
- Mild stimuli are very painful.
- There may be a stabbing component.
- Pronounced summation and after-reaction from stimuli (ie. the pain gets worse with exercise).
This explains why you might feel fine immediately following a car accident, but a week later complain of whiplash. The most common cause of neuropathy is everyday wear and tear or overuse. The significance of this discovery is that disorders such as low back pain, whiplash, frozen shoulder, tennis elbow, fibromyalgia, myofascial pain, and Achilles heel are all physiologically the same.
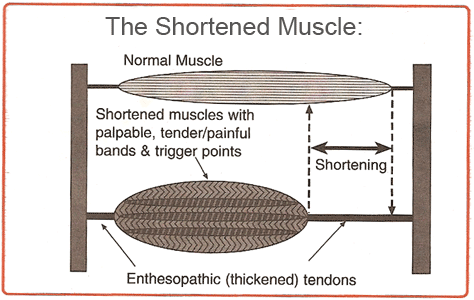
Neuropathy:
Neuropathy is defined as a nerve that is not functioning properly, with or without an altered structure. Damage to the peripheral nervous system is analogous to a supersensitive car alarm.
A common form of neuropathy is myofascial pain. The clinical features of myofascial pain are as follows:
- Continuous, deep, dull aching pain.
- Tender spots (trigger points) in muscles.
- Relief by deactivating trigger points.
- Restricted range of motion in muscles.
- Muscle twitch with trigger point stimulation.
- Patient is startled or jumps with trigger point pressure.
Cannon's Law:
Normal nerve and muscle depend upon intact innervation to provide regulatory or "trophic" effect. It has been shown that any measure which blocks the flow of motor impulses and deprives the effector organ of excitatory input for a period of time can cause "disuse supersensitivity" in that organ, as well as in associated spinal reflexes. Supersensitive nerves and innervated structures react abnormally to stimuli according to Cannon and Rosenbleuth's law of denervation:
"When a unit is destroyed, in a series of efferent neurons, an increased irritability to chemical agents develops in the isolated structure of structures, the effect being maximal in the part directly denervated."
That means, when a nerve is functioning below par and is not functioning properly (neuropathy), it becomes supersensitive and behaves eractically. This principle is fundamental and universal, yet is not well-known or credited. Peripheral neuropathy parallels the aging process, most intense at the weight-bearing and mobility areas of the body.
|
|